You’ve seen specialists, run tests, maybe even been diagnosed with an autoimmune disease like Hashimoto’s, rheumatoid arthritis, or psoriasis. But the treatments only manage symptoms. They don’t answer why this is happening to your body.
The fatigue doesn’t improve with rest, joint pain makes daily tasks difficult, weight gain continues despite diet and exercise, and skin issues won’t clear. If this sounds familiar, you’re not alone. Many people across the Sutherland Shire are searching for answers beyond surface-level symptom management.
Research increasingly suggests that leaky gut syndrome may be a prerequisite for autoimmune disease to develop. Not just a contributing factor, but a necessary condition that must be present for autoimmunity to take hold.
At Happy & Healthy Wellbeing Centre, the gut-autoimmune connection is explored through careful interpretation of functional medicine testing results and targeted naturopathic protocols. Below, we explore how intestinal permeability triggers autoimmune responses, what causes the gut barrier to break down, and how addressing leaky gut may help manage autoimmune conditions.
What Is Leaky Gut Syndrome?
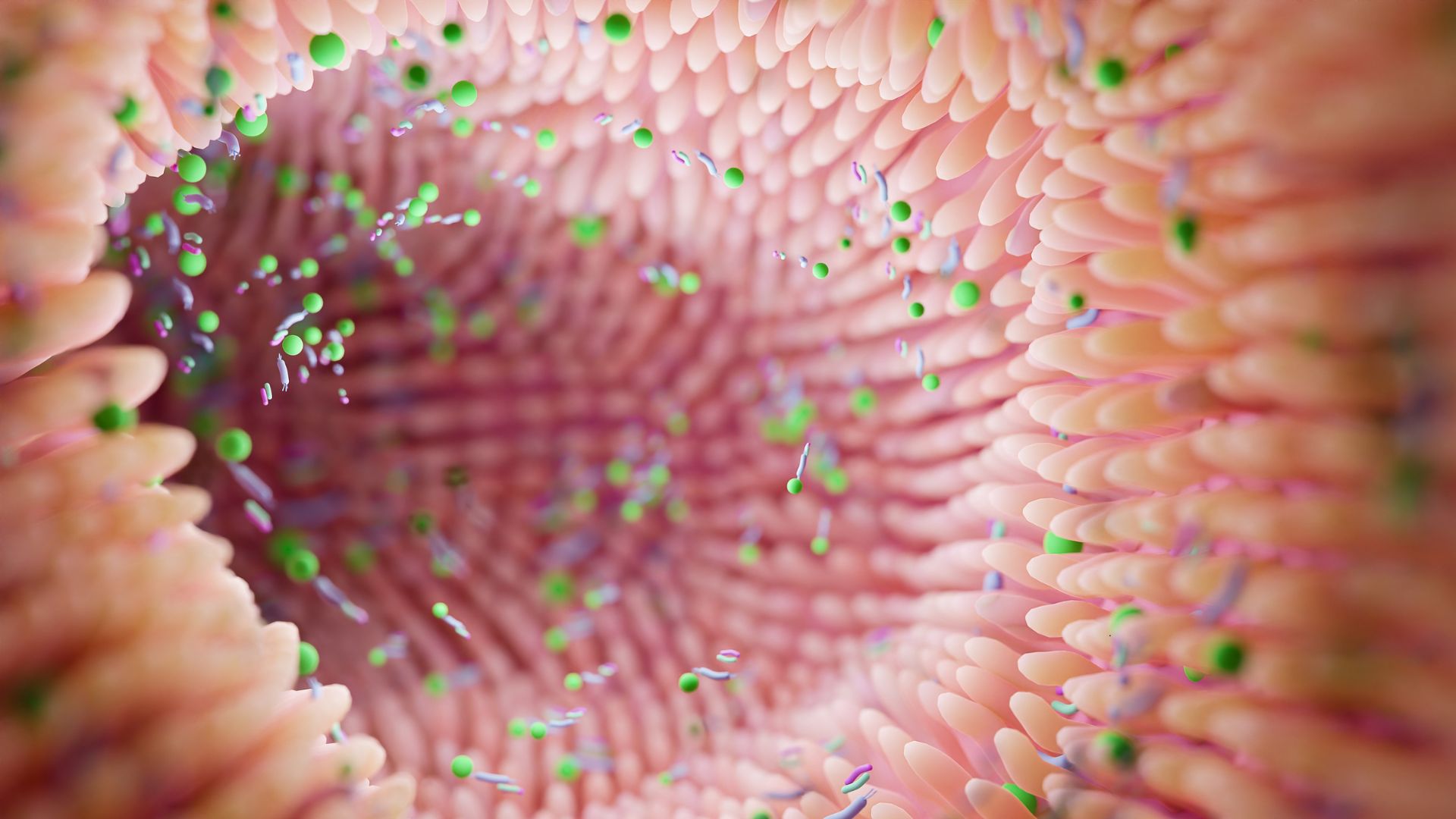
The connection between leaky gut syndrome and autoimmune disease begins with understanding intestinal permeability. Leaky gut occurs when microscopic gaps develop between the cells lining your intestinal wall. The intestinal barrier normally keeps the contents of your digestive system separate from your bloodstream.
Think of your gut lining like a brick wall. When healthy, the intestinal epithelial cells sit tightly together with secure mortar between them. This creates a strong intestinal barrier that controls what enters your bloodstream. With leaky gut, the mortar disappears. Microscopic gaps form in the intestinal barrier that allow unwanted substances to slip through into your body.
The breakdown of intestinal barrier function isn’t about large holes or ulcers appearing in the gut lining. The compromised intestinal barrier function happens at a cellular level, affecting the tight junctions that normally seal intestinal epithelial cells together. These gaps in the intestinal barrier allow partially digested food particles, bacterial fragments, toxins, and larger protein molecules to pass into the bloodstream when they should be moving through and out of the gastrointestinal tract.
Your intestinal lining is only one cell thick. In a healthy gut, intestinal epithelial cells are bound together by tight junction proteins, which act as gatekeepers for the intestinal barrier. A protein called zonulin regulates how open or closed these junctions stay. When zonulin is overproduced, the junctions stay open too long. This increases intestinal permeability, allowing antigens to enter the bloodstream and potentially trigger autoimmune responses.
“Leaky gut” is the term most people use. The medical term for hyperpermeability of the gut mucosa is increased intestinal permeability, or a compromised intestinal barrier. These all describe the same condition where your gut barrier function isn’t working properly. This intestinal barrier dysfunction is central to understanding leaky gut syndrome and the development of autoimmune diseases.
What Causes the Gut Lining to Become Permeable?
Gut Microbiome Imbalances
Your gut contains trillions of bacteria. When balanced, the gut microbiota protects your intestinal lining and regulates immune function. But when harmful bacteria outnumber beneficial bacteria, they produce toxins and inflammatory compounds that directly damage the intestinal barrier.
This bacterial imbalance, called gut dysbiosis (or gut microbiota dysbiosis), is often the primary trigger of leaky gut. The gut microbiome autoimmune disease connection cannot be overstated. Gut bacteria protect and maintain intestinal barrier integrity.
When pathogenic bacteria dominate, they produce lipopolysaccharides that inflame the gut lining, compete with beneficial bacteria for resources, reduce the production of short-chain fatty acids that feed gut epithelial cells, and trigger zonulin release, which opens tight junctions in the intestinal barrier.
This directly contributes to how leaky gut triggers an autoimmune response and develops into an autoimmune disease.
Food Sensitivities and Intolerances
Certain foods trigger immune responses in susceptible people. Some of the most common that can damage the intestinal barrier include:
- Gluten
- Dairy
- Soy
- Sugar
These foods aren’t necessarily inherently bad. But if you’re also stressed or have a disturbed gut microbiome, the proteins in these foods can slip through when there’s too much intestinal inflammation in the gut lining.
Exposure to foods you’re sensitive to creates ongoing inflammation. This gradually damages the intestinal barrier and increases intestinal permeability. The body treats these partially digested food molecules as foreign and mounts an immune response against them, contributing to leaky gut syndrome.
Chronic Stress and Elevated Cortisol

Stress hormones reduce the protective mucus layer in your gut. They divert blood flow away from your digestive system, and they directly compromise tight junctions in the intestinal barrier.
When you’re under too much stress for too long, cortisol itself breaks down proteins, which can cause leaky gut.
This is why stress management isn’t just about mental health. It’s fundamental to healing leaky gut and maintaining intestinal barrier integrity. Chronic stress is one of the main environmental factors that contributes to increased intestinal permeability and autoimmune disease.
Medications
Non-steroidal anti-inflammatories like ibuprofen and aspirin directly damage the gut lining with regular use. These medications have warnings on their labels about not taking them too frequently. Otherwise, you could end up with bleeding of the gut and a compromised intestinal barrier.
Antibiotics wipe out beneficial bacteria along with harmful ones, disrupting the balance of the gut microbiome. This can lead to bacterial overgrowth and opportunistic infections.
Proton pump inhibitors and antacids reduce stomach acid, your body’s first line of defence against pathogens. Without adequate stomach acid, harmful bacteria can survive and thrive, and digestion suffers.
With regular use, these medications contribute to leaky gut and intestinal barrier dysfunction.
Inflammatory Foods
Beyond specific sensitivities, certain foods create intestinal inflammation in most people when consumed regularly:
- Gluten, dairy, sugar, and soy directly damage the intestinal barrier
- Processed foods, additives, and emulsifiers compromise gut barrier function and increase intestinal permeability
- Excess alcohol directly damages the intestinal wall and feeds harmful bacteria in the gut microbiota
All of these contribute to leaky gut syndrome when consumed regularly.
Other Triggers
There are several other factors that damage the intestinal barrier:
- Chronic infections – SIBO (small intestinal bacterial overgrowth), parasites, and Candida overgrowth maintain ongoing intestinal inflammation
- Environmental toxins – Absorbed through food, water, and personal care products, adding to the burden your intestinal barrier must manage
These often compound each other. Stress leads to poor food choices, which leads to intestinal inflammation, which then leads to medication use. It is a downward spiral of gut barrier dysfunction and the start of leaky gut, eventually contributing to autoimmune disease development.
The Gut-Immune System Connection
Understanding the relationship between the gut microbiome and autoimmune disease explains why intestinal health is crucial for immune function.
Approximately 70-80% of your immune system resides in or around your gut. This happens in the gut-associated lymphoid tissue. Your gut is the primary interface between the outside world and your internal body. Everything you eat, drink, or swallow passes through this barrier.
In a healthy digestive system, your gut microbiota trains your immune system from birth. Beneficial bacteria produce anti-inflammatory compounds and teach your immune cells what to attack and what to tolerate. A healthy intestinal barrier allows controlled sampling of the environment, keeping your immune system informed without overreacting.
When this delicate balance is maintained, the immune system can distinguish between harmless substances and genuine threats, reducing the likelihood of chronic inflammation and immune dysfunction that characterise autoimmune conditions.
When bacterial imbalances dominate, you lose this immune regulation. A compromised gut barrier puts your immune system on high alert. Inflammatory signalling becomes chronic rather than occasional, and eventually, your immune system loses its ability to distinguish friend from foe.
Restoring this balance is essential for immune regulation.
How Leaky Gut Triggers Autoimmune Responses
The progression from leaky gut to autoimmune disease follows a predictable pattern.
Step 1: Breach
Undigested food proteins, bacterial fragments, and toxins enter the bloodstream through the permeable gut barrier. Your immune system encounters substances in places they should never be.
Step 2: Immune Activation
Your immune system identifies these substances as foreign invaders and creates antibodies against them. This response is appropriate, as your body is protecting itself.
Step 3: Molecular Mimicry
The real problem starts when leaked proteins resemble your own tissues. Gluten proteins share structural similarities with thyroid tissue. Gliadin in gluten looks like thyroid peroxidase, an enzyme essential for making thyroid hormones.
Your immune system, already on high alert, begins producing antibodies that attack not just the foreign protein but also your own tissues.
Step 4: Chronic Inflammation
Ongoing gut permeability means ongoing immune activation. As more antibodies are produced, more tissue damage occurs, and a self-perpetuating cycle sets in.
Dr Alessio Fasano’s research on zonulin shows that three factors must be present for autoimmune disease to develop: genetic predisposition, environmental trigger, and intestinal permeability.
This means leaky gut isn’t just associated with autoimmunity. It may be a necessary prerequisite. Without the compromised gut barrier, environmental triggers can’t activate the autoimmune process.
By healing the gut, we may be able to halt or even reverse autoimmune progression.
How Leaky Gut Disrupts Hormones and Metabolism
The Liver Connection
When your gut barrier is compromised, bacterial toxins, undigested food particles, and inflammatory compounds flood into your bloodstream. They travel directly to your liver. Your liver is designed to handle a manageable detoxification load. When it becomes overwhelmed with neutralising gut-derived toxins, it has reduced capacity to process hormones.
This leads to hormonal consequences across multiple systems:
- Oestrogen – clearance slows, potentially leading to oestrogen dominance, PMS, and heavy periods
- Testosterone – metabolism is affected, impacting energy, muscle mass, and libido
- Thyroid hormones – conversion from T4 to T3 becomes less efficient
- Cortisol – clearance slows, perpetuating stress hormone elevation
The result is hormonal imbalances that compound your autoimmune symptoms, including fatigue, mood swings, weight gain, and more.
The Weight Gain-Inflammation Cycle
Chronic inflammation from leaky gut triggers insulin resistance. As toxins and bacterial fragments enter the bloodstream, they trigger low-grade inflammation that reduces cells’ responsiveness to insulin. Blood sugar stays elevated after meals, gets stored as fat around your midsection, and triggers intense sugar cravings, which are then followed by energy crashes.
This becomes self-perpetuating. Inflammation drives weight gain, weight gain produces more inflammatory compounds, and these compounds further damage your intestinal barrier.
If you’ve been struggling with unexplained weight gain despite diet and exercise, or hormonal imbalances that don’t respond to treatment, leaky gut may be the underlying cause. This connection is often overlooked in conventional medicine
Common Autoimmune Conditions Linked to Leaky Gut
Research increasingly links intestinal permeability to the development of autoimmune disease.
When patients present with these conditions, it’s reasonable to strongly suspect compromised intestinal permeability at some level. A leaky gut often precedes and contributes to the development of the autoimmune condition.
Multiple autoimmune disorders share this common feature of compromised intestinal barrier function.
| Autoimmune Disease | Leaky Gut Connection | Key Research Findings |
| Hashimoto’s Thyroiditis | Gluten proteins cross the intestinal barrier and trigger antibodies that attack thyroid tissue through molecular mimicry | Elevated zonulin levels found in Hashimoto’s patients; often co-occurs with celiac disease |
| Rheumatoid Arthritis | Gut-derived endotoxins cross compromised intestinal barrier and trigger joint inflammation | Increased intestinal permeability found before diagnosis; linked to Prevotella copri overgrowth |
| Systemic Lupus Erythematosus | Bacterial DNA fragments cross intestinal barrier and activate lupus-specific immune pathways | Bacterial translocation triggers antibody production; healing gut reduces flares |
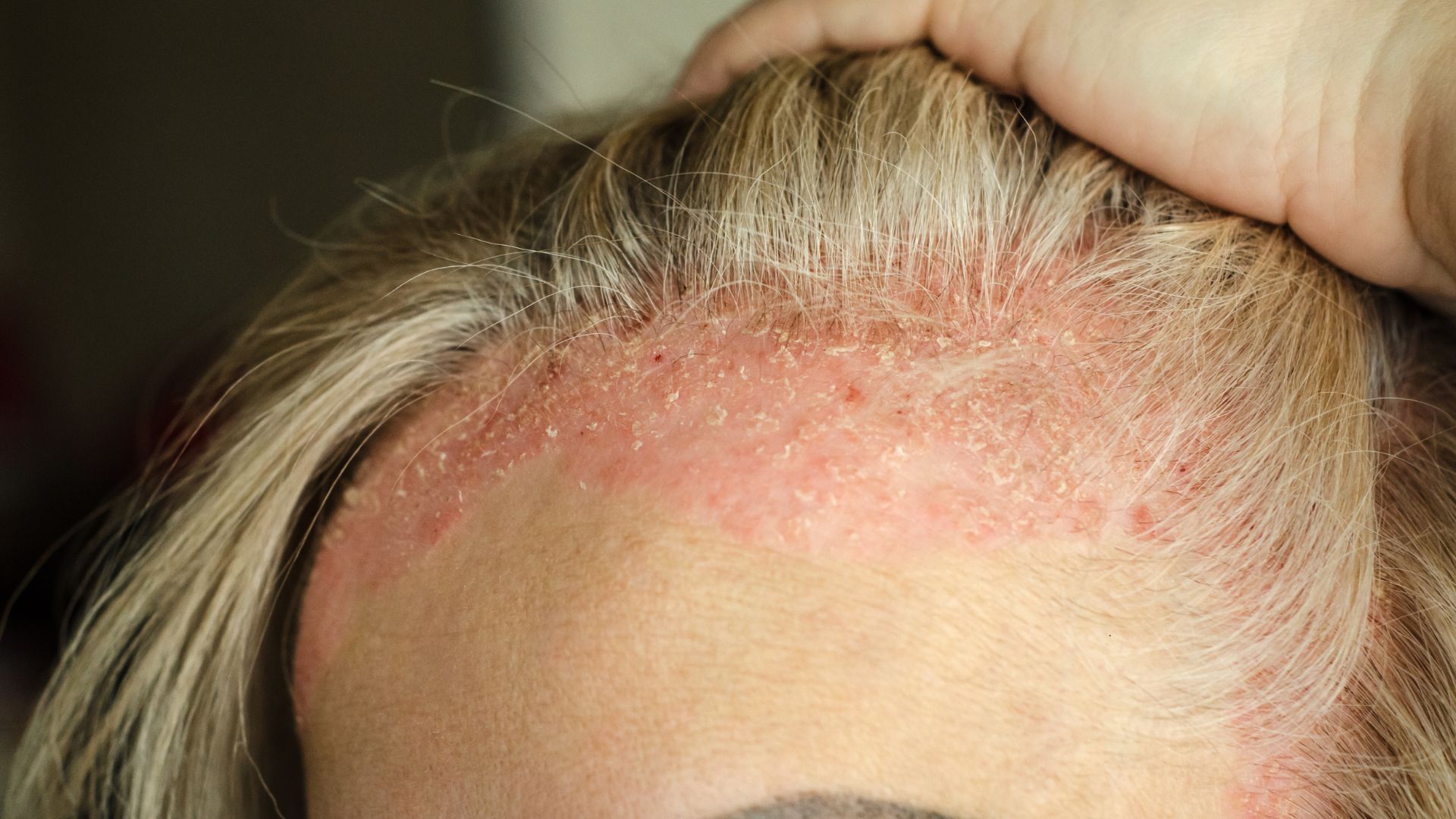
| Psoriasis | Endotoxins from leaky gut trigger skin inflammation | SIBO found in 21% of psoriasis patients with malabsorption; skin clears when gut heals |
| Inflammatory Bowel Disease | Bidirectional – intestinal barrier dysfunction both causes and results from disease | Ongoing intestinal permeability perpetuates inflammation |
| Celiac Disease | Gluten crosses intestinal barrier in genetically susceptible individuals, triggering autoimmune response that damages small intestine | Creates vicious cycle of worsening intestinal permeability |
| Multiple Sclerosis | Gut dysbiosis patterns associated with MS; research suggests possible gut-brain axis involvement | Distinct microbiome composition differences observed in MS patients compared to healthy controls |
Recognising the Signs and Symptoms of Leaky Gut
Leaky gut rarely exists in isolation. Most people experience multiple symptoms spanning digestive, immune, and systemic categories. If several of these resonate with you, it’s worth investigating your gut health.
Digestive Symptoms
Bloating and gas after meals, alternating diarrhoea and constipation, new or worsening food intolerances, abdominal cramping, and undigested food in stool.
Immune and Autoimmune-Related Symptoms
Chronic fatigue unrelieved by rest, brain fog, joint pain or stiffness (especially mornings), skin issues (eczema, rashes, acne, psoriasis), new allergies, recurrent infections, and slow wound healing.
Hormonal and Metabolic Symptoms
Unexplained weight gain (particularly abdominal), difficulty losing weight, blood sugar crashes and cravings, PMS, irregular periods, low libido, hair thinning, and temperature sensitivity.
Mood and Neurological Symptoms
Anxiety, depression, mood swings, sleep disturbances, headaches, and migraines.
When multiple symptoms from different categories appear together, especially alongside diagnosed or suspected autoimmune disease, leaky gut should be investigated. The combination of unexplained weight gain, digestive symptoms, and autoimmune diagnosis is particularly telling.
Testing for Leaky Gut and Autoimmune Connections
At Happy & Healthy Wellbeing Centre in Miranda, comprehensive testing identifies the specific imbalances driving your symptoms. Testing is tailored to your health history and suspected triggers, providing the foundation for effective treatment.
Intestinal Permeability Testing
Lactulose-Mannitol Test
The gold standard for measuring leaky gut. You drink a solution containing two sugar molecules of different sizes. Urine collected over six hours measures how much passes through your gut wall.
Lactulose is a large molecule that shouldn’t cross a healthy intestinal barrier, while mannitol is small and should pass through easily. If lactulose shows up elevated in your urine, it indicates increased intestinal permeability. Your results will generally be available within two weeks.
Zonulin Blood Test
Measures zonulin, the protein that regulates tight junctions. Elevated zonulin indicates active intestinal barrier dysfunction. It is simpler than lactulose-mannitol but less comprehensive and useful for monitoring healing progress over time.
Results show the severity of permeability, whether acute or chronic, and provide a baseline for tracking healing.
Comprehensive Stool Analysis
This test is often more informative than permeability testing alone because it reveals why your gut is leaky.
The test assesses:
- Microbiome diversity and beneficial bacteria levels
- Pathogen screening (parasites, harmful bacteria, yeast/Candida overgrowth)
- Inflammation markers (calprotectin, lactoferrin)
- Digestive function (enzyme production, fat absorption, protein breakdown)
- Immune markers (secretory IgA)
When testing reveals SIBO, parasites, or significant gut dysbiosis, the root cause of the leaky gut becomes clear. Treatment can then be targeted specifically at the underlying infection or imbalance driving the intestinal permeability.
Food Sensitivity Testing
IgG and IgA testing identify delayed immune reactions to foods, which differ from immediate IgE allergies. Common culprits include gluten, dairy, eggs, soy, corn, and nuts.
An important distinction to remember is that food sensitivities are often a consequence of leaky gut. You’re reacting to partially digested proteins entering your bloodstream, not the food itself. As your gut heals, many sensitivities resolve.
Additional Testing
Based on your presentation, additional testing may include:
- Autoimmune antibody panels (ANA, anti-TPO, rheumatoid factor)
- Comprehensive thyroid panel
- Nutrient deficiency testing (B12, iron, vitamin D, zinc)
- SIBO breath testing
- Hormonal panels
Some tests are covered by Medicare (basic antibody panels and thyroid function tests), but functional tests are typically private. Testing recommendations are based on your symptoms and budget, ensuring you get the information you need without unnecessary expense.
Healing Leaky Gut with a Functional Medicine Approach
Healing leaky gut for autoimmune disease requires a comprehensive approach that addresses root causes, not just symptoms. At Happy & Healthy Wellbeing Centre in Miranda, personalised gut-healing protocols and autoimmune treatments are based on test results, symptom patterns, and health goals. Working with a naturopath for leaky gut means access to evidence-based protocols. While every protocol is unique, a proven framework is followed.
The 5R Framework
The 5R Framework is an evidence-based approach for gut restoration.
1. Remove
You can’t heal a wound that’s still being injured. Remove:
- Inflammatory foods (gluten, dairy, sugar, soy)
- Infections and pathogens (parasites, SIBO, Candida, H. pylori)
- Problematic medications where possible (NSAIDs, proton pump inhibitors)
- Stress triggers
This phase typically lasts four to twelve weeks.
2. Replace
Support digestion to prevent larger protein molecules from breaching the intestinal barrier:
- Digestive enzymes (if pancreatic function is compromised)
- Hydrochloric acid support (if low stomach acid)
- Bile acids (for fat digestion)
3. Reinoculate
Restore the protective bacterial community:
- Therapeutic probiotics (specific strains at higher doses)
- Prebiotics (inulin, partially hydrolysed guar gum, resistant starch)
- Fermented foods (sauerkraut, kimchi, kefir, kombucha)
For severe gut dysbiosis or SIBO, probiotic supplementation is delayed until infections clear.
4. Repair
Your intestinal cells regenerate every few days, though complete healing of damaged tissue and restoration of barrier function typically takes six to twelve weeks. Key nutrients include:
- L-glutamine (5-15g daily)
- Zinc carnosine
- Omega-3 fatty acids (EPA/DHA)
- Collagen peptides or bone broth
Gut-healing herbs include slippery elm, marshmallow root, aloe vera gel, and deglycyrrhizinated licorice. Foods like okra, which have a mucousy texture, are often very good for healing the gut.
Dosages are individualised based on testing results.
5. Rebalance
Address lifestyle factors:
- Stress management (vagus nerve activation, adaptogenic herbs)
- Sleep (7-9 hours nightly)
- Moderate exercise
- Toxin reduction
How Long Does Gut Healing Take?

Your intestinal lining has remarkably fast cell turnover; you turn over your gut cells in six to twelve weeks.
Theoretically, you could heal in that timeframe. But practical healing typically requires six months or longer.
The challenge most people face is that they can’t simply separate themselves from their daily life and lifestyle stressors. Realistically, achieving significant change and healing in the gut typically requires at least six months of consistent work, as the intestinal barrier needs time to repair while navigating real-world demands.
Gut cell replacement is just one piece. Gut microbiome rebalancing, immune system recalibration, and changes in stress patterns and dietary habits all take time. The damage may have been accumulating for years.
Most patients notice initial improvements within four to eight weeks with better digestion, increased energy, and reduced bloating. But complete resolution of autoimmune symptoms, such as joint pain and skin issues, and of antibody levels usually takes six to twelve months or longer.
You also need to remember that healing isn’t linear. You’ll have good weeks and setbacks. What matters is the overall trajectory, not day-to-day fluctuations.
Even after active healing, ongoing maintenance prevents relapse. Periodic supplements, mindful eating, and stress management support long-term health.
Foods to Support Gut Healing and Reduce Autoimmune Inflammation
Food is medicine when healing leaky gut. The right foods provide nutrients for tissue repair, fuel beneficial bacteria, and reduce intestinal inflammation. The wrong foods perpetuate gut damage and immune activation.
Foods to Emphasise
| Category | Foods | Benefits |
|---|---|---|
| Collagen & Amino Acids | Bone broth, collagen peptides, slow-cooked meats | Rich in glycine, glutamine, and proline for tissue repair |
| Anti-Inflammatory Fats | Wild-caught fatty fish, extra virgin olive oil, avocados, coconut products | Omega-3s reduce gut inflammation; polyphenols support intestinal lining |
| Fermented Foods | Sauerkraut, kimchi, kefir, kombucha, coconut yogurt | Provide beneficial probiotics for gut microbiota |
| Prebiotic Fibres | Leafy greens, root vegetables, cruciferous vegetables, Jerusalem artichoke, asparagus | Feed beneficial bacteria in gut microbiome |
| Healing Herbs & Spices | Turmeric, ginger, cinnamon, parsley, coriander, basil | Reduce intestinal inflammation and support digestion |
Foods to Avoid
| Category | Foods | Why Avoid |
|---|---|---|
| Gluten | Wheat, barley, rye, spelt, bread, pasta | Triggers zonulin release; molecular mimicry with body tissues |
| Dairy | Milk, cheese, yogurt, butter | Casein protein problematic; lactose intolerance common with intestinal inflammation |
| Sugar & Refined Carbs | White sugar, high-fructose corn syrup, white flour | Feeds pathogenic bacteria and yeast; drives systemic inflammation |
| Soy | Soybeans, tofu, soy milk, soy sauce | Can be inflammatory; often genetically modified |
| Processed Foods | Foods with additives, emulsifiers, preservatives | Damage intestinal lining and gut barrier |
| Vegetable Oils | Canola, soybean, corn oil | High in omega-6; inflammatory |
| Alcohol | All types | Damages intestinal barrier; feeds harmful bacteria |
| Artificial Sweeteners | Aspartame, sucralose, etc. | Alter gut microbiota negatively |
Temporary Eliminations (Individualised)
Some people may need to temporarily avoid grains (even gluten-free), legumes, nightshades, eggs, nuts, or seeds, depending on testing and symptoms.
Your elimination diet will be tailored to your food sensitivity test results, symptom patterns, and autoimmune disease. Many foods initially eliminated can be reintroduced once your intestinal barrier has healed.
Why Work with a Naturopath for Leaky Gut and Autoimmune Conditions
Healing leaky gut and addressing autoimmune conditions requires more than supplements and diet changes. It requires investigation, personalisation, and ongoing support.
How the Approach Differs
Root Cause versus Symptom Management
Conventional medicine excels at diagnosing and managing symptoms of autoimmune disease. Immunosuppressants for inflammation, thyroid medication for Hashimoto’s, and biologics for rheumatoid arthritis can be life-changing and necessary.
But conventional medicine rarely investigates why your immune system is attacking your body in the first place. Naturopathic investigation focuses on upstream factors, including gut permeability, infections, toxin burden, and stress, that trigger the autoimmune cascade.
Functional Testing Access
Most GPs don’t order comprehensive stool analysis, food sensitivity testing, or intestinal permeability testing. These aren’t standard in conventional practice. Specialised functional tests identify specific imbalances driving symptoms.
Time and Individualisation
A typical GP appointment is ten to fifteen minutes. An initial consultation at Happy & Healthy Wellbeing Centre in Miranda is 60 to 90 minutes. This allows time to take a comprehensive health history, connect seemingly unrelated symptoms (such as digestive issues, joint pain, and weight gain), create personalised protocols, and explain why each intervention matters.
Collaborative, Not Alternative
The approach works alongside medical specialists, not instead of them. If you’re on immunosuppressants or thyroid medication, you’re not asked to stop taking them.
Instead, root causes are addressed while you remain on necessary medication. Many patients find they can reduce medications over time as gut healing progresses, always under medical supervision.
What to Expect at Happy & Healthy Wellbeing Centre in Miranda
Your initial 90-minute consultation includes a comprehensive health history, a review of previous test results, a discussion of triggers and patterns, functional testing recommendations, and a preliminary treatment plan.
Follow-up support includes regular check-ins to monitor progress, interpret test results, adjust protocols, and provide guidance on supplements, diet, and meal planning. We troubleshoot challenges as they arise and track improvements together.
Conveniently located in Miranda, we serve patients throughout Sutherland Shire and Southern Sydney.
Take the First Step Toward Understanding Your Symptoms
Living with unexplained autoimmune symptoms is exhausting. The fatigue that never lifts, the weight that won’t budge, joint pain that makes simple tasks difficult, or the frustration when doctors say your tests are normal but you know something is wrong.
The connection between leaky gut and autoimmune disease isn’t speculation. It’s supported by growing scientific evidence. Research suggests that intestinal permeability may be a prerequisite for the development of autoimmune disease, not just a consequence. Many patients with autoimmune diseases have underlying intestinal barrier dysfunction that drives immune dysregulation.
Leaky gut isn’t a life sentence; it’s treatable, and root causes can be investigated, identified, and addressed. When leaky gut is tested for and addressed through comprehensive functional medicine protocols (removing triggers, healing the intestinal lining, and rebalancing the gut microbiota), many patients experience significant improvement in their autoimmune symptoms. While healing typically takes six months or longer, it’s possible.
Your body has a remarkable healing capacity when given the right support. If you’re experiencing autoimmune symptoms, unexplained weight gain, hormonal imbalances, or persistent digestive issues, the naturopaths at Happy & Healthy Wellbeing Centre in Miranda are here to help you investigate the gut-autoimmune connection and create your personalised healing path.
Frequently Asked Questions
Does leaky gut cause autoimmune disorders?
Research increasingly suggests that leaky gut may be a prerequisite for the development of autoimmune disease, not just a symptom. Research shows intestinal permeability must be present alongside genetic predisposition and environmental triggers.
Without the compromised intestinal barrier, environmental triggers cannot activate the autoimmune process. This means healing the gut may halt or even reverse autoimmune progression.
What are the early warning signs of autoimmune disease?
Early signs often include persistent fatigue that is not relieved by rest, joint pain or stiffness (particularly in the morning), skin issues such as rashes or eczema, digestive problems including bloating and food intolerances, brain fog, recurrent infections, and unexplained weight changes.
When multiple symptoms from different body systems appear together, an autoimmune investigation is warranted. Many people experience these symptoms for years before a formal diagnosis.
How do you heal your gut for autoimmune disease?
Gut healing requires a comprehensive approach following the 5R Framework:
- Remove – inflammatory foods, infections, and stress triggers
- Replace – digestive support if needed
- Reinoculate – probiotics and prebiotics
- Repair – L-glutamine, zinc, omega-3s, slippery elm, marshmallow root
- Rebalance – stress management, sleep, lifestyle modifications
This process typically takes six months or longer with consistent adherence to the protocol.
Is it true that 80% of your immune system is in your gut?
Approximately 70-80% of your immune system resides in gut-associated lymphoid tissue. This placement makes sense because your gut is the primary interface between the outside world and your internal body. Your gut microbiome trains your immune system from birth, teaching it what to attack and what to tolerate. When gut health is compromised through bacterial imbalances or increased permeability, immune dysregulation follows, potentially triggering autoimmune responses.

Hayden Keys
Graduating from Western Sydney University in 2005 with a Bachelor of Health Science in Naturopathy, Hayden is a proud member of the Australian Traditional Medicine Society. With over a decade of clinical experience, Hayden established the Happy & Healthy Wellbeing Centre in Miranda in 2009. Read more...




